Health made easier to understand.
Your all-in-one guide to understanding diabetes. Jump to any of the 5 sections below, scroll at your own pace, or tap a dropdown to dig in.
Looking for more information about diabetes? Visit the Diabetes landing page to explore every chapter and topic.
❓ What Is Diabetes?
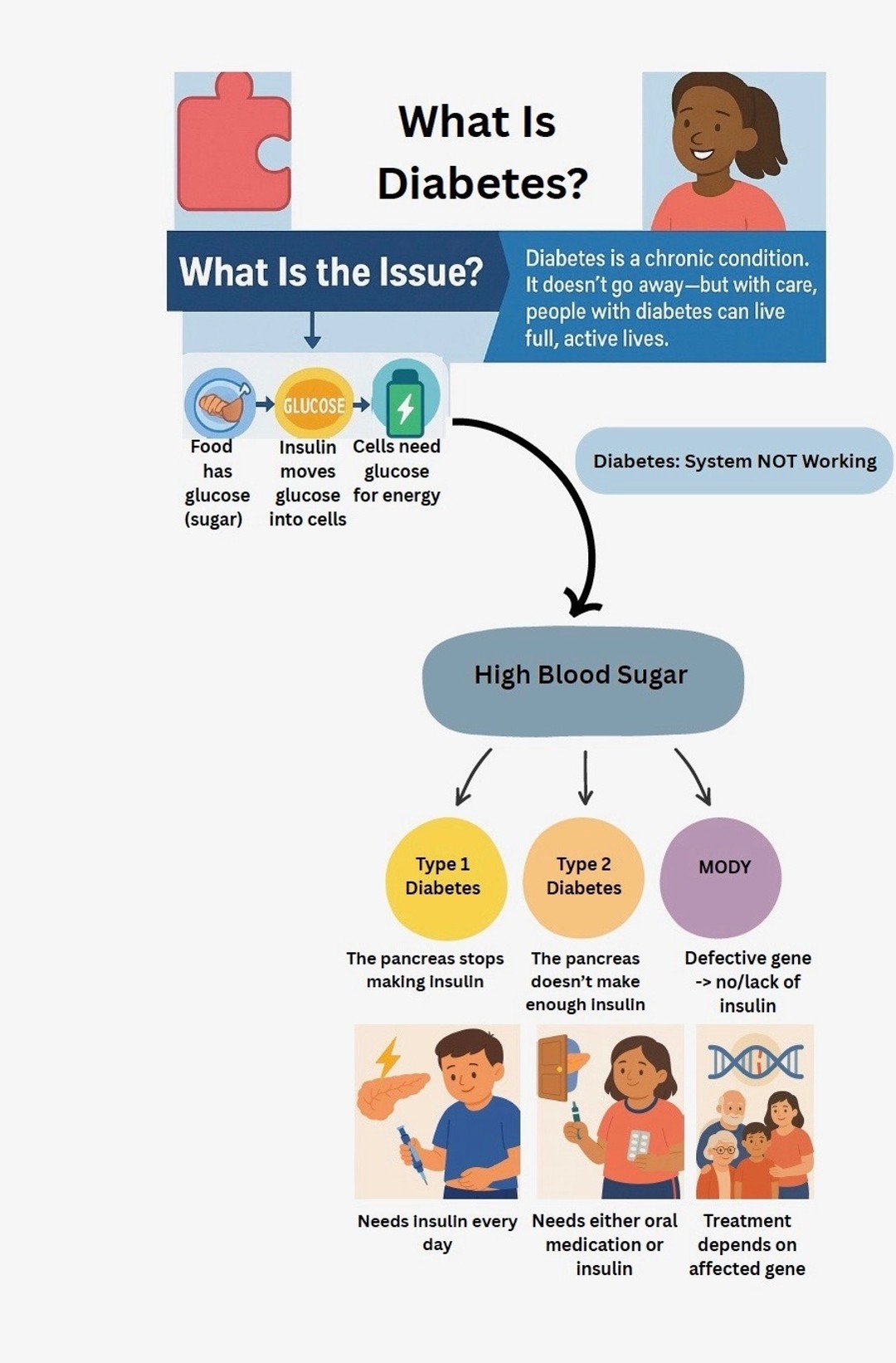
What Is Diabetes?
Open to view the infographic and download it.
📚 Diabetes Types — Quick Review Cards
Diabetes Types — Quick Review Cards
Tap a card to open. Everything is sized for phones—no side-scrolling or squished text.
Type 1 Diabetes (Autoimmune)
Immune system damages insulin-making cells
Type 1 Diabetes (Autoimmune)
Immune system damages insulin-making cells
- Often diagnosed in childhood or adolescence
- Antibodies present in blood tests
- Insulin needed from the start
- Symptoms may start quickly
More
HbA1c is checked every 2–3 months to see how well diabetes is managed.
Type 2 Diabetes (Insulin Resistance)
Body makes insulin but doesn’t use it well
Type 2 Diabetes (Insulin Resistance)
Body makes insulin but doesn’t use it well
- More common in teens; can occur at any age
- No antibodies against insulin-making cells
- Often develops gradually; symptoms may be mild
- Care plan may include healthy habits and medicines
More
Type 2 can affect people of any size. Movement, nutrition, sleep, and medicines help your body respond to insulin.
MODY (Monogenic Diabetes)
Single-gene forms; often run in families
MODY (Monogenic Diabetes)
Single-gene forms; often run in families
- Often diagnosed before age 25
- Seen across multiple generations
- No antibodies; not linked to insulin resistance
- Mutations in a single gene (confirm with genetic testing)
More
Common subtypes include MODY 2 and MODY 3; treatment differs by gene.
 Diagnosing Diabetes – Steps to Diagnosis
Diagnosing Diabetes – Steps to Diagnosis
Diagnosing Diabetes – Steps to Diagnosis
Follow each step. This is a guide for learning only and does not replace care from your healthcare team.
START → Suspect Diabetes?
Symptoms often include increased thirst, frequent urination, fatigue, or unexplained weight loss.
Step 1: Doctor’s Evaluation
Symptom notes, medical & family history, and physical exam.
Step 2: Urine Test
Check for glucose and ketones in urine.
Step 3: Blood Glucose Test
- Fasting glucose ≥ 126 mg/dL → possible diabetes
- Random glucose ≥ 200 mg/dL → possible diabetes
Step 4: HbA1c
HbA1c ≥ 6.5% supports diagnosis (shows 2–3 month average).
Step 5: Optional Oral Glucose Tolerance Test (OGTT)
Use when symptoms are absent/unusual; diabetes if 2-hr glucose ≥ 200 mg/dL.
Step 6: Determine Type
Antibody testing helps tell Type 1 from Type 2. If unclear, consider MODY.
- Autoimmune process
- Insulin needed from onset
- Insulin resistance pattern
- Care may include healthy habits and medicines
- Mild hyperglycemia; strong family history across generations
- No antibodies; not linked to insulin resistance
- Confirm with genetic testing
Step 7: Review & Diagnosis
Doctor reviews physical exam findings and test results together.
🎉 How to Party Smart (Interactive Quiz)
Answer Key & Why
- Q1: B — A balanced meal gives steady energy and reduces later swings.
- Q2: B — Alternating alcohol with water keeps you hydrated and lowers risks.
- Q3: B — Dancing/walking is exercise; it burns glucose and can lower blood sugar.
- Q4: A — A final check plus carbs helps prevent nighttime lows.
- Q5: B — Hydration, breakfast, and glucose check help separate hangover vs. glucose issues.
🩺 Sick Day: What’s Important to Know When You’re Sick — Quick Quiz
Answer Key & Why
- Q1: Your body needs more energy to fight illness — and blood sugar can be harder to manage as a result.
- Q2: Stress hormones like cortisol push blood sugar up, and dehydration from fever, vomiting, or diarrhea adds to the challenge.
- Q3: Most teams suggest checking every 2–4 hours when sick, more often if levels are unstable. Your team will give you your specific frequency.
- Q4: Sip small amounts every 10–15 minutes if you can’t keep much down.
- Q5: Avoid caffeinated drinks — they can worsen dehydration.
- Q6: Fluid choice depends on your blood sugar, ketones, and your team’s plan. Hydration alone doesn’t bring down a high — that’s what insulin is for.
- Q7: True. Small, regular meals or snacks with simple carbs (e.g., Jell-O, popsicles) help keep levels steady. Your team will tell you what’s right for you.
- Q8: Routinely when sick — ketones can rise even when blood sugar looks normal, and they can be an early sign of DKA.
- Q9: Family or friends can check on you and help if your blood sugar drops or you feel worse — important when you’re not feeling well alone.
- Q10: Ketones present means following your team’s sick-day plan and contacting them. Your plan has the exact steps for fluids, insulin, and rechecks.
- Q11: All listed items are red flags — contact your doctor or urgent care immediately.
- Q12: A written sick-day plan from your team — created before you get sick — is the most important thing to have ready. Ask your team if you don’t have one yet.
Important: This quiz is for learning only — not medical advice. Always follow your personal sick-day plan and your medical team’s instructions.
🥦 Nutrition and Carb Quiz
Nutrition and Carb Quiz
Short and interactive.
Look for the Select # badge. It tells you how many correct answers to choose.
Answer Key and Why
- Q1: A, D – A balanced diet helps keep blood sugar steadier and supports overall health and strength.
- Q2: A, B, E – Refined carbs like white rice and pastries and snack foods like chips can cause quicker blood sugar spikes and should be limited.
- Q3: A – A nutritionist helps you understand which foods are healthy, what to limit, how to count carbs, and how to handle eating out or travel.
- Q4: A, B, D – Regular meals and portion control support steadier blood sugar and limiting sugary snacks helps prevent quick spikes.
- Q5: A – Wholegrains digest more slowly, which helps keep blood sugar steadier.
- Q6: A, B – Carb counting helps match insulin doses to food and reduces the risk of very high or very low blood sugar levels.
- Q7: A – When blood sugar is above target, your plan may tell you to round up the dose. Always follow your own team’s instructions.
- Q8: A, B – Food labels and the USDA FoodData Central database help you estimate carbs more accurately.
- Q9 (order): 5, 3, 6, 1, 4, 2 or 5, 2, 6, 3, 4, 1.
Important: This quiz is for learning only, not medical advice. Always follow your personal diabetes plan and your medical team’s instructions.
Calculating Insulin Doses – Challenge
Type your answers as numbers (units). These are practice problems only. Always follow your care team’s plan.
Challenge 1
You plan to eat 50 g carbs. Your ratio is 1 unit per 10 g. How many units do you take?
Challenge 2
You plan to eat 55 g carbs. Your ratio is 1 unit per 10 g and your pre meal blood sugar is higher than target. What is the dose?
Challenge 3
You plan to eat 45 g carbs. Your ratio is 1 unit per 15 g. How many units do you take?
Challenge Answer Key and How to Calculate
- Challenge 1: 50 g ÷ 10 g per unit = 5 units.
- Challenge 2: 55 g ÷ 10 g per unit = 5.5 units. Because your pre meal blood sugar is above target, your plan may tell you to round to 6 units.
- Challenge 3: 45 g ÷ 15 g per unit = 3 units.
Important: These are practice calculations. Your insulin plan is individual. Always follow your medical team’s guidance.
📍 Locations for My Continuous Glucose Monitor (CGM) ⌄
Drag or tap the CGM icons below and place them on the exact body areas where CGMs can be applied.
Copy this into your block:
Pump Placement (Patch vs Tubed)
📦 Patch Pump
How to play: Drag the patches onto the matching teal dots on the figure.

Patch Pump Tips
- Place on soft tissue: upper abdomen, outer thigh, upper-outer buttocks, or back of upper arm.
- Avoid scars, lumps, or spots where clothing rubs.
- Press firmly; let adhesive set before activity or water.
⚠️ Always check your specific device’s Instructions for Use, and when in doubt, ask your diabetes care team before trying a new placement site. Approved pump placement and infusion set sites can vary by brand and by age.
🧪 Tubed Pump
How to play: Drag infusion sets (coral) and pump devices (blue) onto matching dots.

Tubed Pump Tips
- Infusion set on soft tissue (upper abdomen, outer thigh, back of upper arm, upper-outer buttocks).
- Pump device can be clipped to waistband, kept in a pocket, strapped to your leg, or placed between bra cup (girls).
- Route tubing so it won’t snag during sports or sleep.
⚠️ Always check your specific device’s Instructions for Use, and when in doubt, ask your diabetes care team before trying a new placement site. Approved pump placement and infusion set sites can vary by brand and by age.
📱 Scroll Smart: Social Media & Diabetes
Make a choice on each post to reveal a short tip. Tap “Next” to continue.
💛 If you’re struggling and need to talk to someone, tell a trusted adult or contact a youth helpline in your country. Find a helpline near you →
Feeling proud I kept my blood sugar in range today: 105 mg/dL 💪
Quick pic at the park with my device showing. 📍 Central Park
“Lemon water cures diabetes 🍋✨ #LifeHack”
“People with diabetes should just stop eating sugar 😂 #NoExcuse”
“Add me! I’m Mia from Jefferson Middle School—DM me 📱”
“Everyone else has perfect glucose control. I’ll never get it right. 😔”
“This new medication works better than insulin! Link in bio. #Ad”
“Night-time lows are tough. Anyone else?”
Your feed feels heavy today—lots of ads and downbeat posts.
“Check this diabetes website out — looks helpful. #Link”
✅ Taking Charge — Transition Checklist
Knowledge Basics
Nutrition
Social Situations
Sports and Exercise
Medical Appointments & Supplies
Daily Management
Overall Progress
Start checking items to see your progress…
Traveling with diabetes – checklist
Traveling with diabetes doesn’t have to be stressful. With some planning, you can stay safe and enjoy your trip.
